Surgery and Super Pulsed Laser Therapy: 7 Benefits for Patients in Every Procedure
Friday May 28, 2021
By Iker Asteinza, DVM, MSc, Dipl. Small Animal Medicine and Surgery, Animal Home® Veterinary Hospital, Mexico City, Mexico
Veterinary medicine has changed dramatically over the past 10 years in new, unexpected ways. The importance of pets in the daily life of families has increased the demand of the profession. This growth has driven a change in practice, which at times can be stressful, though the goal continues to be enhancing the well-being, recovery, and quality of life for patients. Clients are more committed to their pets than ever and this fuels the desire for veterinarians to discover new and novel treatments to supplement the care provided by medications and surgery. Continuing education, new scientific articles, and emerging technologies need to be considered to help improve patient outcomes and recovery.
Super pulsed laser therapy, a form of low-level laser therapy, has gained much recognition in veterinary medicine due to the results validated in scientific articles for human medicine. In general, laser therapy has been studied more deeply in human medicine and there have been positive outcomes in several areas. Paradoxically, this has often been the way of introducing innovation in veterinary medicine – by transferring uses and therapies in human medicine to establish protocols for animals. It is estimated that in the United States, up to 43 percent of veterinary hospitals already own and use laser therapy devices. Of the remaining hospitals, 20 percent of them refer their patients to hospitals with laser.1
The positive effects of laser therapy in the management of chronic osteoarthritis pain are well known. Laser therapy is non-invasive, easy to perform in the clinic, and has no side effects, which are some of the most popular reasons to prescribe it.1 More veterinarians are recommending laser therapy as part of regular treatment for common diseases: otitis, stomatitis,2 wounds,3 ligament injuries in small animals and horses,4 and corneal ulcers,5 among others.
However, the use of therapeutic laser as a perioperative adjunct and during surgery remains unexplored despite reported results in human medicine. The main benefits following the application of laser therapy include pain management, inflammation reduction, risk reduction of wound infections, and acceleration of tissue repair.6 In many ways, these effects complement surgical procedures; all veterinarians will agree that less pain, reduced use of anti-inflammatories or pain medication, accelerated healing in muscle, bone or skin, and diminished infections help further improve surgical outcomes.
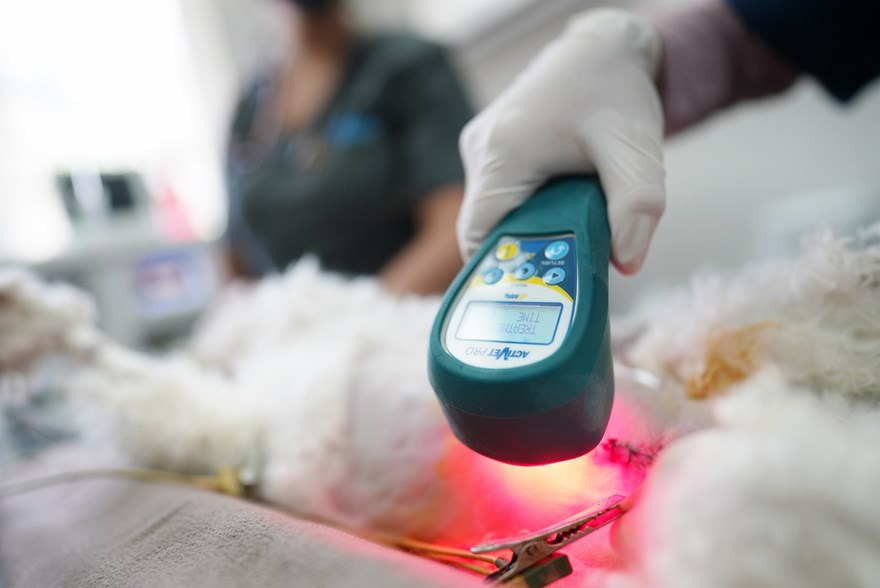
This has led to the inclusion of super pulsed laser therapy (Multi Radiance, Solon, OH) in operative procedures such as:
- dental cleanings
- skin incisions
- wounds
- routine surgeries such as sterilizations
- biopsies
- orthopedic surgeries with osteotomies that require healing of bone, muscle, skin
- inflammation that delays recovery for several weeks
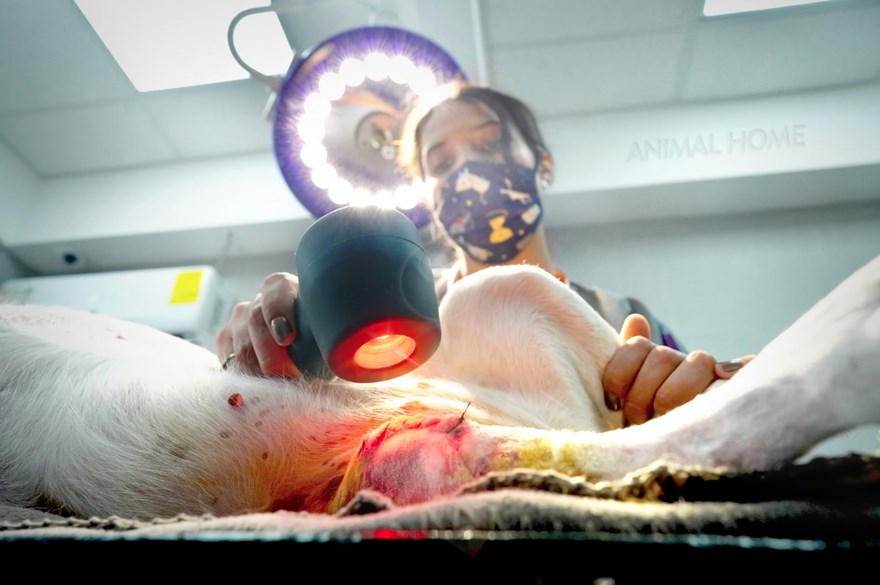
Below are seven ways in which super pulsed laser therapy (Multi Radiance ACTIVet PRO, ACTIVet PRO LaserShower) can improve patient outcomes, enhance everyday procedures, and upgrade veterinary practice.
1. Accelerating Cicatrization
A single dose of light energy at the end of the surgery can surprisingly improve fibrous tissue formation at the wound site by fibroblasts. This is seen not only in the final appearance of the incision, but in the speed of healing in humans7 and in dogs that received laser therapy after hemilaminectomies with better incision appearance and faster healing.8
2. Reducing Pain by Lasing Pre- and Post-Surgery
Pain management has been established as one of the clearest benefits for patients who receive laser therapy. In numerous surgeries and with different times of application, those who received laser therapy prior to undergoing ovarian hysterectomies at specific acupuncture points achieved an analgesic effect that lasted for more than a day with a single treatment.9 Low-level laser also manages to reduce or even eliminate the need for the administration of rescue medications in the first 24 hours after surgery in cats9 and dogs.10
In their 2015 pain management guidelines for dogs and cats, the American Animal Hospital Association and the American Association of Feline Practitioners recommended laser therapy as an effective tool to consider for analgesia.11 Over time, laser therapy’s use as an analgesic has evolved to include traumatic surgeries such as hip arthroplasty; a triple-blinded clinical trial reported reduction of inflammation and pain when standard pain management was complemented with the use of super pulsed laser therapy, decreasing the need to use analgesics and providing greater comfort to patients.12
3. Managing Inflammation: Lasing Pre-, During, or Post-Surgery
In addition to the analgesic influence, another research group reported the anti-inflammatory benefit in molar extractions when performing laser therapy before13 and/or immediately post-surgery14 with positive significant differences for the patients.
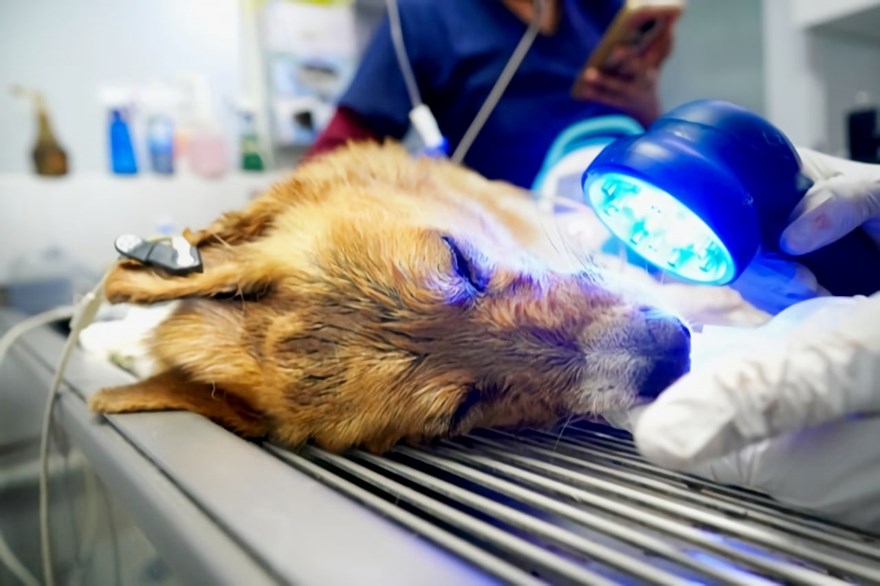
4. Blue Light Kills Pathogens
Blue light exposure can act as an extension of the asepsis typically seen in the first three days after surgery. Its antimicrobial use is helpful in treating pathogens such as the normal flora of the skin or recurrent contaminants. Non-coherent blue light penetrates rather poorly, due to near complete absorption in the superficial layers of the skin. However, that makes it ideally suited to treat conditions of the skin.
Evidence supports the use of blue LED to kill acne,15 MRSA,16 and the bacteria that cause periodontal disease.17 This inclusion offers an entirely new approach to managing wounds by not only accelerating wound repair, but also reducing bacterial burdens of infected wounds. Schnedeker, et al.18 measured the in vitro bactericidal activity of 465 nm blue light (Multi Radiance MR4 ACTIVet PRO) and observed a significant decrease in colony count with blue light irradiation at all doses for MRSA. With the presence of blood as a culture medium in any surgery wound, these could complicate any surgery. The use of blue light must be considered.
5. Improving Bone Healing and Regeneration
Therapeutic laser for surgery is also known to promote angiogenesis, improvement of blood flow, release of ATP, and stimulation of growth factors, fibroblasts, and biomarkers. These are natural promoters of regeneration not only at the superficial plane, but also in muscle tissue, bone, and deep tissue, in addition to promoting cell differentiation in bone formation.19
Therefore, the use of super pulsed laser therapy should be considered for orthopedic surgeries that require bone formation such as osteosynthesis for fractures, tibial tuberosity advancement (TTA), triple pelvic osteotomy (TPO), and tibial plateau leveling osteotomy (TPLO), knowing that super pulsed laser therapy is free of thermal effects and safe to use with metal implants.
In neurological surgeries, such as hemilaminectomy in patients with compression due to intervertebral disk disease (IVDD), the use of laser therapy has shown a quicker recovery, achieved by ambulation three to four times faster than the control group; this is advantageous because ambulatory dogs have a lower incidence of urinary tract infections, pneumonia, disease muscle atrophy, and decubital ulcers.20
6. Improving Rehabilitation Outcomes
After surgery, specifically in rehabilitation, super pulsed laser therapy has shown great benefits to control pain, regenerate tissue, and strengthen muscles and ligaments.21 In the first three to five days after surgery, the focus is reducing inflammation and pain, as well as stimulating vascularization and healing. Laser therapy is recommended after healing has been achieved to restore normal joint movement through the strengthening of muscles.22
7. At-Home Care: Same Results with Less Stress for Pets and Owners
Post-op care is of utmost importance, sometimes requiring daily laser therapy treatments. Patients and owners may have difficulty returning to the clinic for this continued therapy. Rental laser therapy devices (Multi Radiance My Pet Laser) allow pet owners to administer treatments to pets in the comfort of home, under the direction of the veterinarian.
Home-based treatments are an easier and convenient option for both pets and pet owners; devices are simple to operate, and at-home therapy reduces the stress of traveling for multiple clinic visits. A rental program allows veterinarians to reduce the burden patient care and generate passive income for the practice. Veterinary practices can offer the latest technology while showing concern for the well-being of patients.
Conclusion
Veterinary surgical procedures are necessary but can come with complications. Utilizing laser therapy before, during, and after surgery can reduce pain, control inflammation, and accelerate wound healing in patients, reducing the burden of patient care. Veterinarians should consider adding this non-invasive, safe modality to their daily surgical procedures to enhance patient outcomes and improve their practices.
Iker Asteinza Castro, MVZ M.SC. Dipl. Small Animal Medicine and Surgery, has more than 20 years of experience and owns two reference veterinary hospitals in Mexico City, Mexico. He lectures on laser therapy in international congresses, as well as the benefits of laser therapy in the everyday practice. View his Laser Therapy U webinar on Veterinary Surgery and Super Pulsed Laser.
References
- Barger BK, Bisges AM, Fox DB, Torres B. Low-Level Laser Therapy for Osteoarthritis Treatment in Dogs at Missouri Veterinary Practice. J Am Anim Hosp Assoc. 2020 May/Jun;56(3):139-145. doi: 10.5326/JAAHA-MS-6851. Epub 2020 Mar 17. PMID: 32182110.
- Khaleel Ahmed M, Jafer M, Nayeem M, et al. Low-Level Laser Therapy and Topical Medications for Treating Aphthous Ulcers: A Systematic Review. J Multidiscip Healthc. 2020;13:1595-1605. Published 2020 Nov 18. doi:10.2147/JMDH.S281495
- Evans DH, Abrahamse H. Efficacy of three different laser wavelengths for in vitro wound healing. Photodermatol Photoimmunol Photomed. 2008 Aug;24(4):199-210. doi: 10.1111/j.1600-0781.2008.00362.x. PMID: 18717961.
- Zielińska P, Nicpoń J, Kiełbowicz Z, Soroko M, Dudek K, Zaborski D. Effects of High Intensity Laser Therapy in the Treatment of Tendon and Ligament Injuries in Performance Horses. Animals. 2020; 10(8):1327. https://doi.org/10.3390/ani10081327
- Rhee Y, Cho KJ, Ahn J, Chung P. Effect of Photobiomodulation on Wound Healing of the Corneal Epithelium through Rho-GTPase. Medical Lasers 2017;6:67-76. https://doi.org/10.25289/ML.2017.6.2.67
- Lindsay Hochman, Photobiomodulation Therapy in Veterinary Medicine: A Review, Topics in Companion Animal Medicine, Volume 33, Issue 3, 2018, Pages 83-88, ISSN 1938-9736, https://doi.org/10.1053/j.tcam.2018.06.004
- Friedman O, Gofstein D, Arad E, Gur E, Sprecher E, Artzi O. Laser pretreatment for the attenuation of planned surgical scars: A randomized self-controlled hemi-scar pilot study. J Plast Reconstr Aesthet Surg. 2020 May;73(5):893-898. doi: 10.1016/j.bjps.2019.11.046. Epub 2019 Dec 16. PMID: 31926893.
- Wardlaw JL, Gazzola KM, Wagoner A, et al. Laser Therapy for Incision Healing in 9 Dogs. Front Vet Sci. 2019;5:349. Published 2019 Jan 29. doi:10.3389/fvets.2018.00349
- Nascimento FF, Marques VI, Crociolli GC, Nicácio GM, Nicácio IPAG, Cassu RN. Analgesic efficacy of laser acupuncture and electroacupuncture in cats undergoing ovariohysterectomy. J Vet Med Sci. 2019;81(5):764-770. doi:10.1292/jvms.18-0744
- Tomacheuski RM, Taffarel MO, Cardoso GS, et al. Postoperative Analgesic Effects of Laserpuncture and Meloxicam in Bitches Submitted to Ovariohysterectomy. Vet Sci. 2020;7(3):94. Published 2020 Jul 21. doi:10.3390/vetsci7030094
- Epstein ME, Rodanm I, Griffenhagen G, Kadrlik J, Petty MC, Robertson SA, Simpson W; AHAA; AAFP. 2015 AAHA/AAFP pain management guidelines for dogs and cats. J Feline Med Surg. 2015 Mar;17(3):251-72. doi: 10.1177/1098612X15572062. PMID: 25701863.
- Langella LG, Casalechi HL, Tomazoni SS, Johnson DS, Albertini R, Pallotta RC, Marcos RL, de Carvalho PTC, Leal-Junior ECP. Photobiomodulation therapy (PBMT) on acute pain and inflammation in patients who underwent total hip arthroplasty-a randomized, triple-blind, placebo-controlled clinical trial. Lasers Med Sci. 2018 Dec;33(9):1933-1940. doi: 10.1007/s10103-018-2558-x. Epub 2018 Jun 16. PMID: 29909435.
- Petrini M, Ferrante M, Trentini P, Perfetti G, Spoto G. Effect of pre-operatory low-level laser therapy on pain, swelling, and trismus associated with third-molar surgery. Med Oral Patol Oral Cir Bucal. 2017;22(4):e467-e472. Published 2017 Jul 1. doi:10.4317/medoral.21398
- Eroglu CN, Keskin Tunc S. Effectiveness of Single Session of Low-Level Laser Therapy with a 940 nm Wavelength Diode Laser on Pain, Swelling, and Trismus After Impacted Third Molar Surgery. Photomed Laser Surg. 2016 Sep;34(9):406-10. doi: 10.1089/pho.2016.4101. Epub 2016 Jul 15. PMID: 27420732.
- Morton CA, Scholefield RD, Whitehurst C, Birch J. An open study to determine the efficacy of blue light in the treatment of mild to moderate acne. J Dermatolog Treat. 2005;16(4):219-23. doi: 10.1080/09546630500283664. PMID: 16249142.
- Enwemeka CS, Williams D, Enwemeka SK, Hollosi S, Yens D. Blue 470-nm light kills methicillin-resistant Staphylococcus aureus (MRSA) in vitro. Photomed Laser Surg. 2009 Apr;27(2):221-6. doi: 10.1089/pho.2008.2413. PMID: 19196103.
- Chui C, Hiratsuka K, Aoki A, Takeuchi Y, Abiko Y, Izumi Y. Blue LED inhibits the growth of Porphyromonas gingivalis by suppressing the expression of genes associated with DNA replication and cell division. Lasers Surg Med. 2012 Dec;44(10):856-64. doi: 10.1002/lsm.22090. Epub 2012 Nov 5. PMID: 23129157.
- Schnedeker AH, Cole LK, Lorch G, Diaz SF, Bonagura J, Daniels JB. In vitro bactericidal activity of blue light (465 nm) phototherapy on meticillin-susceptible and meticillin-resistant Staphylococcus pseudintermedius. Vet Dermatol. 2017 Oct;28(5):463-e106. doi: 10.1111/vde.12451. Epub 2017 May 22. PMID: 28543810.
- Amid R, Kadkhodazadeh M, Ahsaie MG, Hakakzadeh A. Effect of low level laser therapy on proliferation and differentiation of the cells contributing in bone regeneration. J Lasers Med Sci. 2014 Fall;5(4):163-70. PMID: 25653816; PMCID: PMC4281990.
- Draper WE, Schubert TA, Clemmons RM, Miles SA. Low-level laser therapy reduces time to ambulation in dogs after hemilaminectomy: a preliminary study. J Small Anim Pract. 2012 Aug;53(8):465-9. doi: 10.1111/j.1748-5827.2012.01242.x. Epub 2012 Jul 11. PMID: 22783835.
- Flaherty MJ. Rehabilitation Therapy in Perioperative Pain Management. Vet Clin North Am Small Anim Pract. 2019 Nov;49(6):1143-1156. doi: 10.1016/j.cvsm.2019.07.006. Epub 2019 Aug 28. PMID: 31473030.
- Baltzer, "Rehabilitation of companion animals following orthopedic surgery," N Z Vet J., vol. 68, no. 3, pp. 157-167, May 2020.



